 Clear Choice Laser is now offering corneal cross-linking procedures using the KXL® System, the first and only FDA-approved therapy for progressive keratoconus. The machine, created by Avedro, was approved in April, along with Avedro’s Photrexa® Viscous and Photrexa® solutions, and is being used in about 100 facilities nationwide.
Clear Choice Laser is now offering corneal cross-linking procedures using the KXL® System, the first and only FDA-approved therapy for progressive keratoconus. The machine, created by Avedro, was approved in April, along with Avedro’s Photrexa® Viscous and Photrexa® solutions, and is being used in about 100 facilities nationwide.
What is Keratoconus?
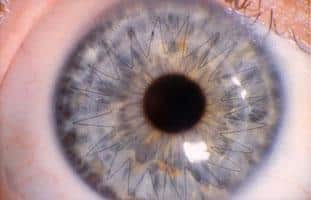
Keratoconus is a common eye disease that occurs in approximately 1 in 750 Americans. In this condition, the cornea becomes weak, progressively thinner, and irregular in shape which can cause high levels of astigmatism. Instead of a normal, relatively round shape resulting in clear vision, the cornea in keratoconus can become cone shaped. This can interfere with the ability to see clearly. Often keratoconus patients first require glasses, then contact lenses, and, if the condition progresses to a severe level, a corneal transplant may be required.
Treating Keratoconus with Corneal Cross-Linking
This system is used to treat keratoconus, a condition in which the cornea (the front clear window of the eye) becomes weak, thin, or irregularly shaped. Corneas with keratoconus can bulge forward into a cone shape, causing poor vision. It affects 1 in 750 Americans, and while the preliminary stages simply necessitate glasses, eventually the condition may require a corneal transplant.
The KXL® System facilitates corneal collagen cross-linking, a keratoconus treatment that has been in use since 1998. It combines the use of ultraviolet light and riboflavin to strengthen collagen fibrils on the cornea. This makes the cornea more rigid, and less likely to worsen over time.
Our Corneal Cross-Linking Procedure
The Corneal Cross-linking keratoconus treatment is an outpatient procedure performed in the doctor’s office using numbing eye drops and a valium tablet. After numbing drops are applied to the eye, the epithelium (the thin layer on the surface of the cornea) is gently removed. Photrexa Viscous eye drops will be applied to the cornea for at least 30 minutes. Depending on the thickness of your cornea, Photrexa drops may also be required. The cornea is then exposed to UV light for 30 minutes while additional Photrexa Viscous drops are applied.
Qualifying for Corneal Cross-Linking
To qualify for the keratoconus treatment, patients’ corneas cannot be too thinned or too scarred for the procedure. During your consultation, we will determine if Corneal Cross-linking might be an option for you. Our practice offers a complimentary, no touch, painless, screening test to see whether Corneal Cross-linking might help you.
Would you like to be contacted about Corneal Cross-linking?
Would you like to download a brochure to learn more about Corneal Cross-linking?
Frequently Asked Questions
What is astigmatism?
Astigmatism means that the front surface of the eye (the cornea or clear window in front of the eye) is less round and more irregular in shape so the image won’t focus clearly on the retina in the back of the eye. This can result in poor vision and glare.
What does Corneal Cross-linking do?
Normal corneas have crosslinks between its collagen fibers that keep it strong and able to retain its normal shape. In keratoconus, the cornea is weak with too few cross-links or support beams. This weakened structure allows the cornea to bulge outwards. The cross-linking keratoconus surgery adds cross-links or “cross beams” to the cornea, making it more stable, holding its shape and focusing power better. These new cross-links help strengthen the cornea which stops the thinning process and further loss of vision.
Should your relatives be tested?
As you may know, keratoconus is a condition that often runs in families, so it’s important to arrange a screening for all family members of patients with keratoconus. If caught early, there is a good chance that keratoconus surgery can halt the progression of keratoconus and prevent the need for uncomfortable contact lens wear and/or corneal transplant.
How effective is Corneal Cross-linking?
Many research studies have shown that Corneal Cross-linking may prevent further vision loss in over 95% of patients and improves vision in 60-81% of patients treated. 1-11
Is Corneal Cross-linking like LASIK?
No. LASIK is a procedure that reduces or, in some cases, may even eliminate the need for glasses or contact lenses by removing corneal tissue. The Corneal Cross-linking keratoconus treatment does not remove tissue. The purpose of Corneal Cross-linking is to prevent further deterioration of vision for most patients and to potentially improve vision. Patients will typically require a lower eyeglass prescription or can have an easier time being fit with contact lenses.
Can Corneal Cross-linking prevent the need for corneal transplant?
Many studies have shown that keratoconus surgery can often prevent the need for a corneal transplant and allow patients to wear contact lenses or glasses more comfortably and safely again. 1-11
Can a corneal transplant be done after Corneal Cross-linking?
If Corneal Cross-linking does not prevent the need for a corneal transplant, then a corneal transplant can generally be performed.
Can I have Corneal Cross-linking if I already had a corneal transplant?
Each patient and each patient’s eyes are different. In some cases Corneal Cross-linking can be performed after corneal transplantation.
What’s the difference between a corneal transplant and Corneal Cross-linking?
Corneal Cross-linking keratoconus treatment is an in office procedure that does not involve surgical incisions into the eye or stitches. It is a relatively non-invasive procedure that is done with vitamin drops and light. Corneal transplants are performed in an operating room, involving incisions into the eye and a lifelong risk of rejection of the corneal tissue.
Is Corneal Cross-linking new?
Corneal collagen cross-linking has been performed since 1999. The results and safety profile of Corneal Cross-linking have been very positive in numerous studies throughout the world. In fact, by September of 2006, Corneal Cross-linking had been approved by all 25 European Union nations. Corneal Cross-linking procedures are now routinely performed on patients as young as 10 years old in Europe to prevent the development of keratoconus.
Does Corneal Cross-linking need to be repeated?
In many studies, the majority of patients responded to a single vitamin and light Corneal Cross-linking treatment and did not need to have the procedure repeated. Corneal Cross-linking can often be repeated when treatment is not effective.
What is the transepithelial (or epi-on) Corneal Cross-linking technique?
In this less invasive keratoconus treatment, the surface skin layer (epithelium) of the cornea is not removed so the recovery is much faster than the traditional Corneal Cross-linking technique. This less invasive technique can only be done on corneas that are thicker than 400 microns12,13. Your surgeon will be able to determine if you might be a candidate for transepithelial Corneal Cross-linking treatment.
How long does the procedure take?
If two eyes are being treated at once, the procedure takes approximately an hour and a half. If only one eye is being treated at a time, the procedure takes approximately one hour.
Does the Corneal Cross-linking procedure hurt?
No. The cross-linking procedure is painless. Anesthetic eye drops are used to avoid any discomfort during the procedure. Some patients have some discomfort after the procedure and your surgeon can tell you whether you are or are not likely to do so.
Can I have one eye treated at a time?
Yes, your doctor will discuss the advantages and disadvantages of treating one eye or two eyes at a time.
When is the best time to have Corneal Cross-linking?
As with most conditions, prevention of a problem is better than treatment of a problem. The best time for keratoconus treatment is before astigmatism has become severe and vision has been lost. This does not mean that people with very poor vision from keratoconus cannot be helped by Corneal Cross-linking. However, the results of Corneal Cross-linking for patients with advanced keratoconus have not been as good as for patients with early disease.
If Corneal Cross-linking works for me and stops my vision from getting worse, can I have laser vision correction or Intacs afterwards?
Some patients may be able to have an excimer laser treatment (PRK) or Intacs to improve their vision without glasses after they have healed from the Corneal Cross-linking procedure.
Do I have to stop wearing contacts before having Corneal Cross-linking?
We recommend that you stay out of contact lenses for a week or two if possible before your consultation visit to see if you might benefit from the investigational Corneal Cross-linking procedure. This can vary based on how difficult it is for you to see without your contacts. We often suggest patients not wear their lenses for 3 days before their Corneal Cross-linking procedure.
When can I resume wearing contact lenses?
Most patients can return to wearing contact lenses 2 to 6 weeks after having the cross-linking procedure depending on whether you are a candidate for transepithelial Corneal Cross-linking. Your surgeon will determine how long this might take in your case.
Will I need new glasses or contacts after Corneal Cross-linking?
Because cross-linking often improves vision, patients find that their old contacts or glasses are too strong for them and they need to be refit with new, glasses and/or contact lenses. Most of the time, patients can wear their old glasses until several months after the procedure when their doctor will prescribe new ones. Because the effects of Corneal Cross-linking occur slowly, patients don’t generally have to change their glasses very often.
When will I notice any improvement in my vision after Corneal Cross-linking?
With the traditional Corneal Cross-linking procedure, most patients find that immediately after the keratoconus treatment, their vision is actually worse than it was before the procedure. This usually goes on for roughly 3-6 weeks. Patients may start to notice positive effects 4-8 weeks after the procedure and may experience major improvement in vision at least 3-6 months after the investigational procedure. In some studies patients’ vision and astigmatism were still continuing to improve five years after the cross-linking procedure2 so visual improvement is a long process. With the less invasive transepithelial Corneal Cross-linking, some patients found their vision improved as early as several weeks after treatment.
When can I exercise and return to my usual activities after Corneal Cross-linking?
We want to help you be able to work or do other things you need and want to do as quickly as possible. Based on the type of Corneal Cross-linking procedure, your doctor can tell you when you can return to your usual activities. With traditional Corneal Cross-linking, most people can usually do so after 5-7 days. With transepithelial Corneal Cross-linking, most people return to their usual activities the next day.
Does insurance cover Corneal Cross-linking?
Because of the regulatory environment in the US, this procedure is investigational so Corneal Cross-linking treatment is not covered by insurance.
Some insurances cover Corneal Cross-linking. Your vision counselor will help you to submit to insurance so that we can receive a response on if your procedure is covered, and what out of pocket costs you have, if any.”
References:
- Wollensak G, Spoerl E, Seiler T.; Riboflavin/ultraviolet-a-induced collagen crosslinking for the treatment of keratoconus. AJO 2003 May;135(5):620-7
- Raiskup-Wolf F, Hoyer A, Spoerl E, Pillunat LE.; Collagen crosslinking with riboflavin and ultraviolet-A light in keratoconus: long-term results. J Cataract Refract Surg. 2008 May;34(5):796-801.
- Coskunseven E, Jankov MR 2nd, Hafezi F.; Contralateral eye study of corneal collagen cross-linking with riboflavin and UVA irradiation in patients with keratoconus.
J Refract Surg. 2009 Apr;25(4):371-376
- Grewal DS, Brar GS, Jain R, Sood V, Singla M, Grewal SP.; Corneal collagen crosslinking using riboflavin and ultraviolet-A light for keratoconus: one-year analysis using Scheimpflug imaging. J Cataract Refract Surg. 2009 Mar;35(3):425-32.
- Spoerl E, Mrochen M, Sliney D, Trokel S, Seiler T.; Safety of UVA-riboflavin cross-linking of the cornea. Cornea. 2007 May;26(4):385-9.
- Trattler W, Rubinfeld R, Corneal Collagen Cross-linking; Cataract and Refractive Surgery Today; September 2009
- Caporossi A, Mazzotta C, Baiocchi S, Caporossi T. Long-term Results of Riboflavin Ultraviolet A Corneal Collagen Cross-linking for Keratoconus in Italy: The Siena Eye Study. Am Journal of Ophthalmology 2010:149:585-593 www.ajo.com/article/S0002-9394(09)00808-3/abstract
- Raiskup-Wolf F, Hoyer A, Spoerl E, Pillunat LE. Collagen crosslinking with riboflavin and ultraviolet-A light in keratoconus: long-term results. J Cat Ref Surg. 2008
- Vinciguerra P, Albè E, Trazza S, Seiler T, Epstein D. Intraoperative and postoperative effects of corneal collagen cross-linking on progressive keratoconus. Arch Ophth. 2009
http://archopht.ama-assn.org/cgi/content/abstract/127/10/1258
- Daley, R. Cornea
Cross-linking vision improvement evidence mounts. Eyeworld, 2010. http://www.eyeworld.org/article.php?sid=5268&strict=&morphologic=&query=Daley, R. Corneal%26%238232%3BCross-linking vision improvement evidence mounts.
- Rubinfeld RS, Trattler WB, Martin NF, Adi MA and The CXL-USA Study Group: Answering Your Patients’ Questions About Cross-Linking; Advanced Ocular Care. March 2010:25-28
bmctoday.net/advancedocularcare/2010/03/article.asp
- Boxer Wachler BS, Pinelli R, Ertan A, Colin CKC. Safety and efficacy of transepithelial crosslinking (C3-R/CXL), J CATARACT REFRACT SURG – VOL 36, Pgs 186-187, JANUARY 2009
- Pinelli R, El Beltagi T, Leccisotti A. Update on Corneal Crosslinking. Cataract and Refractive Surgery Today October 2008: 67-69. http://www.crstodayeurope.com/Issues/1008/1008_19.php
 Clear Choice Laser is now offering corneal cross-linking procedures using the KXL® System, the first and only FDA-approved therapy for progressive keratoconus. The machine, created by Avedro, was approved in April, along with Avedro’s Photrexa® Viscous and Photrexa® solutions, and is being used in about 100 facilities nationwide.
Clear Choice Laser is now offering corneal cross-linking procedures using the KXL® System, the first and only FDA-approved therapy for progressive keratoconus. The machine, created by Avedro, was approved in April, along with Avedro’s Photrexa® Viscous and Photrexa® solutions, and is being used in about 100 facilities nationwide.












